Research by
Nicole Harlan, John Kappelman, Reuben Reyes, (The University of Texas at Austin)
and
Stewart Veeck (Howmet Research Corporation)

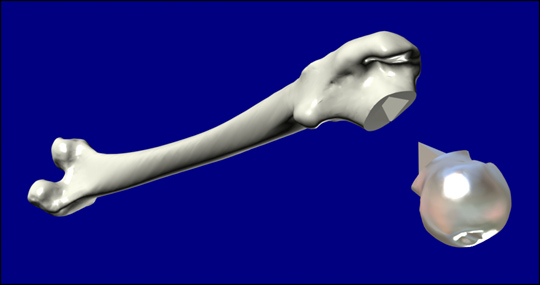
A portion of a human bone was replicated in titanium to demonstrate that the complex surface of an actual bone could be recreated in a structural implant material. Although titanium is currently used for bone replacement, implants are simple geometric approximations of the bone shape. Mismatches between implants and real bone often cause stress concentrations and result in premature implant failure. In this project, an accurate digital model of a bone was sliced into discrete layers. A reproduction of the bone was constructed using Selective Laser Sintering (SLS), a layered manufacturing process developed at The University of Texas at Austin. Rapid prototyping technologies such as SLS are ideal for producing complex parts and prototypes because no specific tooling or patterns are required. Because the titanium piece is an exact duplicate, it will fit the patient's bone structure exactly and have a longer service life.
In this study, an accurate titanium replica of the ball section of a human
femur bone was produced. The major limiting factor in titanium processing
is the metal's extreme reactivity with many atmospheric elements, particularly
at elevated temperature. To avoid titanium contamination a mold for
titanium casting, rather than the implant itself, was produced using SLS.
Titanium was then cast into the mold using standard methods, thereby maintaining
a low level of metal contamination. The key aspect of the project was the
selection and development of a mold material system that could withstand the
titanium casting process and could be produced using Selective Laser Sintering.
Nicole Harlan, a Ph. D. student in the Materials Science
& Engineering Program and a member of the Laboratory for Freeform Fabrication, was
the principle investigator of the project. She coordinated all aspects of
the project and developed the method to make zirconia-based molds for titanium
casting.
The complete process was complicated and required the effort of several
different entities. Special acknowledgements are given to Professor John
Kappelman and the eSkeletons
Project in the Department of Anthropology, to Reuben Reyes in the
ASE/EM Learning Resource Center, and
to Stewart Veeck at the Howmet
Research Corporation.
The processing steps included:
| 1) Acquiring a
very detailed 3D representation of the outer surface of a human
femur 2) Generating a 3D model of the bone that could be manipulated digitally 3) Creating and modifying a 3D digital mold of the ball section of the femur 4) Constructing and post-processing zirconia mold material 5) Characterizing and refining the production process 6) Creating a usable bone mold and casting at a titanium foundry 7) Evaluating the integrity of the finished titanium pieces |
Details of each step involved in the process are in explained below.
1. A human femur bone from the Anthropology Department
collection was 3D laser scanned at the Physical Anthropology computer lab.
The resulting data was a very accurate representation of the superficial
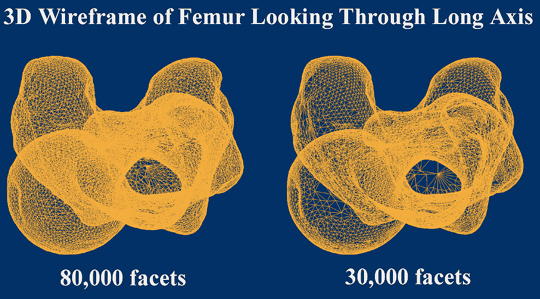
topographic features of the bone. The initial 3D data set contained
80,000 facets and retained a high degree of accuracy. However, a data set
of this size is generally too large to work with and had to be reduced.
Below is an image of the Digibotics 3D laser scanning machine used to scan the
human femur.

2. The 3D digital data was transferred to the UT
ASE/EM LRC to be digitally processed. The original 3D digital model was
too complex to manufacture using the laser-sintering machine available at UT.
Thus, the first step was to reduce the number of facets representing the
femur bone to 30,000 while maintaining part accuracy. The 3D digital
model was then sectioned by digitally separating the ball section from the shaft
of the femur. A locator peg was added to the ball section to indicate
where it would contact the shaft portion of the femur.
3. The ball section and peg were inverted to create
a digital mold. This was a rather complex process because the mold
geometry had to meet the specifications of the titanium foundry. The size
and shape of the neck, where molten titanium would enter the mold, had to be
shaped to prevent pressure build-up and ensure proper metal flow. In
addition, a small vent hole was added to allow the titanium to completely fill
the mold. Finally, to conserve material, the size of the mold was reduced
by 50 percent. The finished 3D digital mold was converted to an STL
format so it could be constructed in a Selective Laser Sintering workstation.
Below are 3D computer images of the making of the digital mold in various
stages.

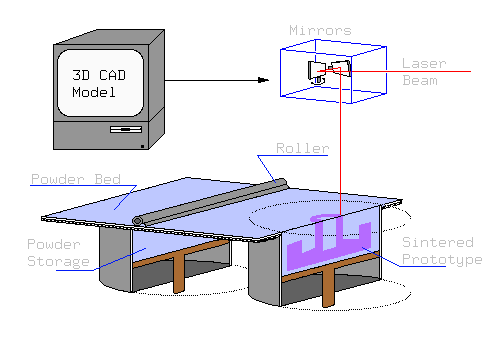
4. Samples of mold material were built on an SLS
Model 125 Workstation, located in the Laboratory for Freeform Fabrication
(Mechanical Engineering Department). The base material was a mixture of
stabilized zirconia powder and a sacrificial polymer binder. During
post-processing, the sacrificial polymer binder was replaced by unstabilized
zirconia and the material was fired to increase strength. Below is a
diagram of the laser sintering machine.
5. Strength, roughness and shrinkage were measured on
material samples before and after each processing step. The values
obtained were used to refine the process. Shrinkage could be accurately
predicted, and roughness and strength were brought to acceptable levels for
titanium casting. Below are two sets of femur and ball inserts made in
nylon with the Selective Laser
Sintering process.

6. A simple test mold and two molds of the bone
section were made in the SLS Workstation from the digital models and
post-processed. The molds were taken to Howmet
Research Corporation, a foundry in Whitehall, Michigan, to be cast with
titanium. Below are 3 computer images of the final digital mold.

7. The titanium castings were prepared
metallographically. Optical microscopy revealed a thin alpha case on the
surface of the casting, typical of as-cast titanium alloys. The thickness
of the alpha case was comparable to those obtained using standard mold
materials. Roughness measurements indicated an as-cast surface roughness
(Ra) of 8 microns. Below are pictures of cast titanium (dark)
and broken zirconia molds (white).

It is hoped that a damaged bone can be replaced with a customer-specific
titanium implant using the outlined production method. An X-ray, CT or
MRI scan of a symmetric, non-damaged bone could be reversed and used to
construct the mold for a damaged bone. Essentially any damaged bone (a
finger, toe, hand, arm, foot, jaw, or skull) could be replicated in a titanium
implant. The high strength to weight ratio and biocompatibility of
titanium make it a reliable implant material, and now, using digitally designed
zirconia molds, better fitting implants can be produced.


Project Participants/ Collaborators:
Dr. Nicole Harlan,
Dr. John Kappelman,
Stewart Veeck,
Special thanks to Adam Kalmbach (undergraduate researcher) and SeokMin Park
(Ph. D. student, Mechanical Engineering) for their assistance in producing the
molds.
Web Acknowledgment:
Publications:
Proceedings:
Talks:
Want to see more... 3D models...
Animations.